The heart’s ability to beat in a regular, coordinated rhythm depends entirely on a precise electrical system. When that system fails — whether from age, disease, or damage — the heart may beat too slowly, pause unexpectedly, or lose its coordination entirely. A pacemaker is a small, implantable device that takes over the role of the heart’s natural electrical system, delivering carefully timed electrical impulses to keep the heart beating safely and effectively.
At Vikram Heart Care Centre, pacemaker implantation and long-term device management are provided by Dr Kushaal Vikram, bringing specialist cardiac rhythm expertise to patients in Patna and the wider Bihar region.
Understanding the Heart’s Electrical System
Before understanding why a pacemaker is needed, it helps to understand how the heart’s electrical system works under normal conditions.
Every heartbeat begins with an electrical impulse generated by the sinoatrial (SA) node — a small cluster of specialised cells in the upper right chamber of the heart (right atrium). This natural pacemaker fires at a rate of 60 to 100 times per minute at rest, sending an impulse that spreads across both atria, causing them to contract and push blood into the ventricles.
The impulse then reaches the atrioventricular (AV) node — a relay station between the upper and lower chambers — which briefly delays the signal before passing it to the ventricles via the Bundle of His and Purkinje fibres. This delay allows the ventricles to fill completely before they contract, pumping blood out to the lungs and body.
When any part of this system is damaged or diseased, the heart may beat too slowly (bradycardia), pause, or fail to coordinate properly — with potentially serious consequences for the patient.
What Is a Pacemaker?
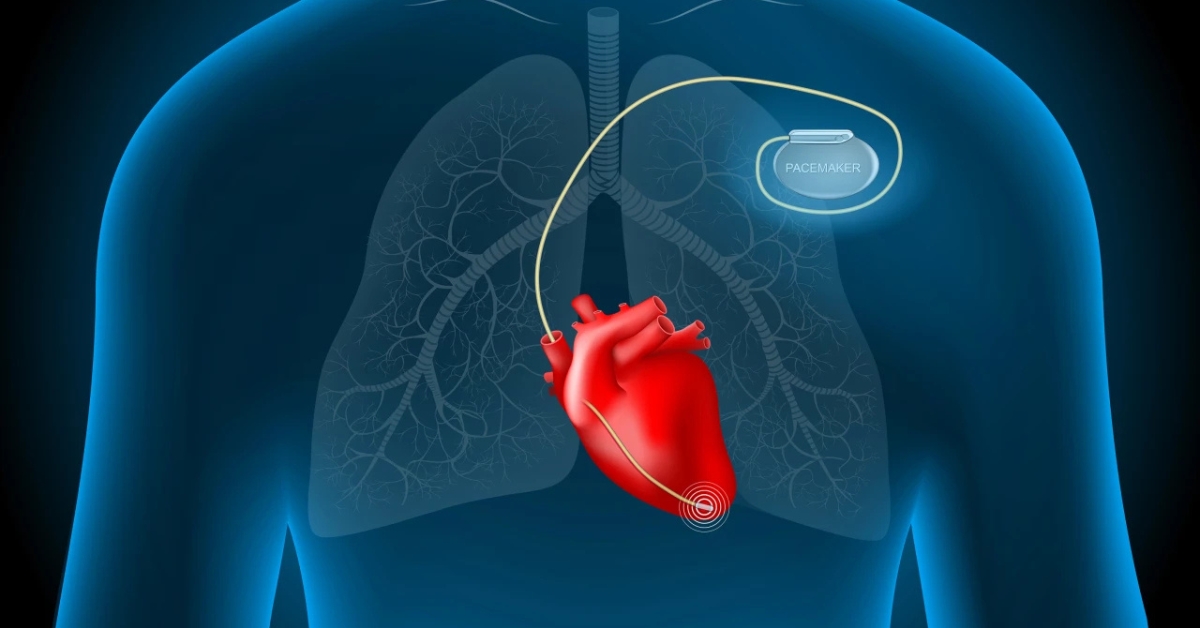
A pacemaker is a small battery-powered electronic device, roughly the size of a large coin, implanted beneath the skin of the chest. It consists of two main components:
The pulse generator — a sealed unit containing the battery and the electronic circuitry that controls timing and delivers impulses.
The lead or leads — thin, insulated wires that connect the pulse generator to the heart muscle. They carry electrical impulses from the device to the heart and also sense the heart’s own natural electrical activity.
Modern pacemakers are sophisticated devices that continuously monitor the heart’s electrical activity and only deliver a pacing impulse when needed — if the heart’s own rate falls below a programmed threshold. They adapt their pacing rate to the patient’s level of physical activity through built-in motion sensors, ensuring an appropriate heart rate during both rest and exercise.
Types of Pacemakers
Single-Chamber Pacemaker Has one lead, positioned either in the right ventricle or, less commonly, the right atrium. Used for specific types of heart block or sinus node dysfunction.
Dual-Chamber Pacemaker Has two leads — one in the right atrium and one in the right ventricle. This allows the device to coordinate timing between the upper and lower chambers, more closely mimicking the natural sequence of the heartbeat. The most commonly implanted type for most bradycardia indications.
Rate-Responsive Pacemaker Incorporates sensors that detect physical activity or breathing rate and adjust the pacing rate accordingly. Recommended for patients who are physically active or those whose heart rate does not increase normally with exercise.
Cardiac Resynchronisation Therapy (CRT) Device A specialised type of pacemaker with three leads — right atrium, right ventricle, and left ventricle — used in patients with heart failure and abnormal ventricular conduction (typically left bundle branch block). By coordinating the contraction of both ventricles simultaneously, CRT improves the heart’s pumping efficiency and can significantly improve symptoms and quality of life in selected patients.
Implantable Cardioverter-Defibrillator (ICD) Combines pacemaker function with the ability to detect and treat life-threatening fast rhythms (ventricular tachycardia and ventricular fibrillation) by delivering a controlled shock to restore normal rhythm. Recommended for patients at high risk of sudden cardiac death.
Leadless Pacemaker A newer generation miniaturised pacemaker that is implanted directly inside the right ventricle via a catheter through the femoral vein, with no leads and no chest pocket. Suitable for selected patients where a conventional pacemaker carries a higher complication risk.
Conditions Requiring a Pacemaker
A pacemaker is recommended when the heart’s electrical system is not functioning adequately to maintain a safe and sufficient heart rate.
Sick Sinus Syndrome (Sinus Node Dysfunction) The SA node — the heart’s natural pacemaker — fires too slowly, pauses, or alternates between abnormally slow and fast rates. Symptoms include fatigue, dizziness, fainting, and exercise intolerance.
Heart Block Disruption of electrical conduction between the atria and ventricles at the level of the AV node or below.
- First-Degree Heart Block — delayed conduction; usually does not require pacing
- Second-Degree Heart Block (Mobitz Type I / Wenckebach) — progressive delay until a beat is dropped; may or may not require pacing depending on symptoms and degree
- Second-Degree Heart Block (Mobitz Type II) — unpredictable dropped beats without preceding delay; higher risk of progression to complete block; usually requires pacing
- Third-Degree (Complete) Heart Block — no conduction between atria and ventricles; the ventricles beat at a very slow escape rhythm; requires permanent pacing
Bundle Branch Block with Syncope Bifascicular or trifascicular block with symptoms of syncope or pre-syncope may indicate intermittent complete heart block and warrant pacemaker implantation.
Chronotropic Incompetence An inability of the heart rate to increase appropriately in response to exercise or physiological demand, causing significant exercise intolerance.
Hypersensitive Carotid Sinus Syndrome and Vasovagal Syncope Selected patients with recurrent fainting episodes related to carotid sinus hypersensitivity or vasovagal syncope with a significant cardioinhibitory component may benefit from pacemaker implantation.
Post-Cardiac Surgery or Ablation Temporary or permanent pacemakers may be required following cardiac surgery or catheter ablation procedures that affect the conduction system.
The Implantation Procedure
Pre-Procedure Assessment
Before implantation, a thorough cardiac evaluation is performed including ECG, echocardiogram, blood tests, and in some cases electrophysiology study to confirm the indication and plan the appropriate device and lead configuration.
The Procedure
Pacemaker implantation is performed in a cardiac catheterisation laboratory under local anaesthesia with sedation. General anaesthesia is not usually required.
The steps involved:
- A small incision is made just below the collarbone, typically on the left side
- The lead or leads are inserted through the subclavian or cephalic vein and guided under X-ray (fluoroscopic) guidance into the correct position within the heart
- Lead position is tested to confirm adequate sensing and pacing thresholds
- The leads are secured and connected to the pulse generator
- The pulse generator is placed in a small pocket created beneath the skin below the collarbone
- The incision is closed with sutures
The procedure typically takes 1 to 2 hours depending on the complexity and number of leads. Most patients are admitted for an overnight stay and discharged the following day after a device check and chest X-ray to confirm lead positions.
Post-Procedure Care
- The arm on the side of the implant should not be raised above shoulder height for 4 to 6 weeks to allow the leads to stabilise in position
- Avoid heavy lifting, strenuous upper body activity, and contact sports during the healing period
- The wound should be kept dry and clean
- A pacemaker identification card will be issued — carry it at all times
- Notify all healthcare providers and airport security of your pacemaker
Pacemaker Follow-Up and Device Management
A pacemaker is not a once-and-done intervention — it requires regular monitoring throughout its operational life.
Routine follow-up includes:
- Device interrogation — a non-invasive check performed with a programmer placed over the device; assesses battery status, lead function, pacing and sensing thresholds, and stored cardiac events
- Review of arrhythmia logs stored in the device memory
- Reprogramming of pacing parameters if required based on clinical needs
- Battery life monitoring — modern pacemakers typically last 7 to 15 years depending on usage; battery replacement requires a minor procedure to replace the pulse generator while retaining the existing leads
Remote monitoring — many modern devices can transmit data wirelessly to the clinic between scheduled visits, allowing early detection of device issues, arrhythmias, or clinical deterioration.
Living With a Pacemaker
The vast majority of patients with a pacemaker lead full, active lives with minimal restrictions. Understanding a few practical considerations helps ensure the device functions safely.
Electromagnetic interference: Most household appliances — televisions, microwaves, computers, mobile phones — do not interfere with modern pacemakers. However, certain medical and industrial equipment can:
- MRI scanning — many modern pacemakers are MRI-conditional; discuss with your cardiologist before any MRI scan
- Diathermy (surgical cautery) — inform your surgical team of your pacemaker before any procedure
- Transcutaneous electrical nerve stimulation (TENS machines) — seek cardiology advice before use
- Strong industrial magnets and arc welding equipment
Mobile phones: Keep mobile phones at least 15cm away from the pacemaker site. Do not carry a phone in a breast pocket on the same side as the device. Normal use including calls and texts is otherwise safe.
Travel and airport security: Inform airport security staff of your pacemaker before passing through security scanners. Carry your pacemaker identification card. Body scanners at airports are generally safe but hand-held security wands should not be held directly over the device for a prolonged period.
Exercise and physical activity: Most patients with pacemakers can exercise normally. Rate-responsive pacemakers automatically increase the pacing rate during physical activity. Discuss specific activities with Dr Kushaal Vikram.
Frequently Asked Questions
Q: Will I feel the pacemaker working?
Most patients do not feel the pacing impulses delivered by a modern pacemaker. Some patients who were very symptomatic before implantation simply notice that their previous symptoms — fatigue, dizziness, or breathlessness — have resolved. Occasionally, patients who are entirely pacemaker-dependent at high rates may be aware of pacing, but this is uncommon.
Q: How long does a pacemaker battery last?
Battery life depends on how frequently the pacemaker is pacing and the programmed output settings. Most modern pacemakers last between 7 and 15 years. The battery is monitored at every follow-up visit and replacement is planned well in advance of actual depletion. Battery replacement is a minor procedure involving only replacement of the pulse generator — the existing leads are retained in most cases.
Q: Can I have an MRI scan with a pacemaker?
Many modern pacemakers are MRI-conditional — meaning they can be safely scanned under specific conditions with appropriate precautions. Older devices may be contraindicated for MRI. Always inform your radiologist and cardiologist before any MRI scan so that the device can be checked, temporarily reprogrammed if necessary, and monitored during the scan.
Q: Will I need to restrict my activities after getting a pacemaker?
During the first 4 to 6 weeks after implantation, you should avoid raising the arm on the implant side above shoulder height and avoid heavy lifting or strenuous upper body activity to allow the leads to stabilise. After this healing period, most normal activities including exercise can be resumed. Contact sports and activities involving direct impact to the device site should be discussed with your cardiologist.
Q: Is there a risk of the pacemaker failing?
Modern pacemakers are extremely reliable. Serious device failures are rare. However, lead-related issues — such as lead displacement (more likely in the first few weeks), lead fracture, or insulation break — can occasionally occur and are detected during routine follow-up. This is why lifelong device monitoring is essential.
Q: Can a pacemaker be removed if it is no longer needed?
Pacemaker explantation is technically possible but is a more complex procedure than implantation, particularly for leads that have been in place for many years as they can become adherent to the vessel wall and heart tissue. It is generally only undertaken when there is a specific clinical reason such as infection. In most cases, a pacemaker is considered a permanent implant.
Q: I have been told I need a pacemaker but I feel fine. Do I really need it?
Some pacemaker indications — particularly complete heart block — are based on the documented severity of the electrical abnormality and the risk of progression rather than current symptoms alone. A patient with complete heart block may feel relatively well on an escape rhythm but is at significant risk of cardiac arrest without pacing. Your cardiologist will explain the specific reason for the recommendation in your case.
Q: Is pacemaker implantation available in Patna?
Yes. Pacemaker implantation and long-term device management are available at Vikram Heart Care Centre, Dr K K Kantha Memorial Hospital, Patna, under the care of Dr Kushaal Vikram.
Book a Consultation
If you have been experiencing unexplained dizziness, fainting, extreme fatigue, or have been told you have a slow heart rate or heart block, a specialist cardiac evaluation is the essential next step.
📞 +91 893 583 4142 | +91 886 400 4584
📍 21 B/3, Patliputra Colony, Near Pataliputra Golambar, Opp. UNICEF Building, Patna 800 013
🌐 Book online at kanthahospital.com

